
Services
Downloads
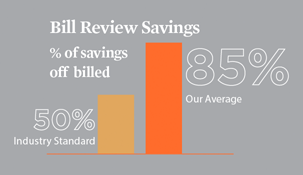
Bill Review
Marquee’s bill review services bring value to our clients because we are able to provide transactional speed and accuracy, improved operations, productivity, compliance and medical and administrative savings with our customized bill review system.
Our tailored software is customizable to provide ultimate flexibility for our client-driven rules and fee schedule rules.
- Bill reviewers certified by department of insurance
- Multi–state and multiple lines of business experience
- Multi–line bill review
- Out of network negotiation
- Ability to support Network Partnerships for our clients both prospective and retrospectively with PPOs/Specialty Networks/PBMs to optimize network utilization and increased savings.
- Integration with utilization review – only certified treatment is processed and paid.
- Intelligent bill review detects potential provider fraud
- Ability to load client custom routing rules
- Complex bill reviews routed to senior bill reviewer
- Nurse Audit Review – validate injury relatedness, complexity of services billed, unbundling of services, match services to Precertification/ Authorizations.
Another way we’re meeting our clients’ needs – A bill review system that is customized to their needs.
Clinical Management Solutions
Perfecting The Medical Management Balancing Act
Helping injured workers return to work while managing the costs for our clients has become our specialty.
An automated online referral process ensures our dedicated preferred vendors are used. Our online processes include:
- Case management
- Customizable reporting
- Client notification
Board Certified Medical Review Staff
- Occupational Medicine
- Orthopedics for spine, hand, and general ortho–surgery
- Pain Management
- Dentistry
- Psychiatry
- Physical Medicine & Rehabilitation (PM&R)
- Chiropractic
- Neurology
- Gastroenterology
Marquee Managed Care Solutions offers proven solutions to medical cost containment while highlighting customized strategies for our clients.
Utilization Review
We have highly skilled licensed nurse clinicians who deliver timely treatment decisions with the most updated online California State/Regulatory Guidelines available at their fingertips. We offer full service Utilization Review which is fully integrated with our bill review application. We offer the following state certified services:
- Contract negotiation with non-fee schedule entities i.e., Functional Restoration Programs, Skilled Nursing-Long Term Care Facilities, Acute Rehab inpatient
- Prospective reviews
- Concurrent reviews
- Retrospective reviews
- Physician advisor/peer review
Compounded/Narcotic Medication Review
We offer quality clinical opinions on medications whether there is a concern for abusive prescribing patterns or the focus is on high dollar spend with opioid usage. We have an on-staff pharmacy doctor, as well as medical doctors specializing in pain management for review of medical records, drug utilization review, and narcotic control program. All these programs have a focus on improved clinical outcome and financial benefit to the claim. The narcotic program was developed to address inappropriate opiate use and to develop alternatives for the injured employee, while staying within the confines of treatment related to the claim.
Telephonic Case Management & Early Return to Work
Our team of registered nurses is highly experienced and educated in case management for the California Workers’ Compensation market as well as other state jurisdictions with medical management and discharge planning coordination. Their mission is to oversee care by directing the claim to affect positive outcomes for the injured employee as well as the employer. Registered nurses apply appropriate state mandated guidelines in conjunction with extensive medical experience to move the claim along, avoiding missed opportunities to capture savings. Through early entry management of a claim, our nurses can drive medical care and provide predictive modeling for who are likely candidates to return to work.
Specialist Panel
Nurses
- Discharge planning coordination
- Contract negotiation with rehabilitation facilities, skilled nursing facilities, functional restoration programs
- Develop return to work plan with employers and physicians for employees early entry back–to–work with cost savings
- Work with employees, employers and medical providers to create a cost–reducing return–to–work plan
- Aggressive cost containment practices
- Utilization Review RN medication review for high–dollar cases
- Claims request review-only
Physicians
- Utilization Peer Review
- Peer–to–Peer contact
- On–site educational programs for claims staff
- Case conference by phone
- Medication review
Field Case Management
Recognizing the value of face to face contact with catastrophically injured employees can go a long way in providing that caring touch which may resonate with benefits to the claim, such as enhancing return to work. We partner with the best national vendors to deliver this service.
Our nurses are all licensed RNs and case managers with experience in:
- Brian injury
- Cardiology
- Disability management
- Neurological diseases
- Orthopedics
- Spinal cord injuries
Role of Physician Advisor & Peer Review
When requested treatment falls outside state guidelines, the utilization review nurse sends the case to our physician advisors for peer review. Treatment requests are matched to the best physician for the case and follow evidence based medicine and State Guidelines in applying a peer decision. If the case needs clarification, our nurses will facilitate communication with appropriate parties (requesting physician, claims adjuster, or the clinical nurse manager).
Our physicians go a step further and will offer their services to look at the claim, provide physician advisory reviews which help the claims examiner to determine disability management issues, such as compensability, return to work, and narcotic opioid management. The overall benefit is to focus on moving the claim along to return to work and reducing costs along the way.
Negotiation Resolution
With more than 90 years of combined industry experience, the Negotiations & Resolution Unit (NRU) has vast and varied knowledge that lends to a versatile, comprehensive approach and unrivaled strategies for tough lien resolution. Our industry-wide recognition and relationships facilitate the best settlements for our clients. We have a proven track record showing greater medical cost savings and lower defense costs on NRU files.
Specialized Services
- Lien negotiations
- Out-of-network and complex bill review negotiations
- Hearing representative services
- Expert bill review witnesses
Lien Negotiations
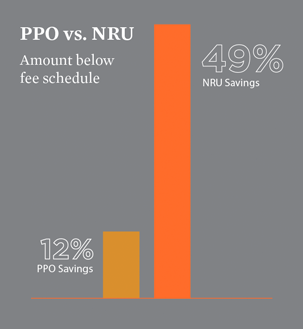
Averaging savings in excess of 49% below fee schedule, our expert team of designated negotiators maximizes its efforts via telephonic services for more immediate results. Each negotiator has a solid reputation within the industry that drives further success and achieves more equitable settlements. Our fees are outcome based, which result in a greater incentive for overall program savings.
Out–of–Network Negotiations & Custom Bill Review Negotiations
This service was specifically designed to assist clients when medical services are obtained outside of a customized savings network. Our experts focus on minimizing the high dollar out-of-network hospital bills, rehabilitation admissions (pre-admission or post-discharge) and reducing allowances on fee schedule exclusions such as dental, transportation and interpreting bills. Our negotiation services are not limited to the above as we are always working to assist our clients in achieving the most optimal savings possible in order to reduce potential loss costs.
Hearing Representative Services
With more than 90 years of combined industry expertise and knowledge, our team of experts specializes in lien hearings/trials, walk-through settlements and provides thorough cost benefit analysis (ROI) of litigation vs. settlement to provide maximum savings. NRU hearing representative services, combined with our competitive and flexible program pricing options, allow for immediate and significant savings results unmatched by traditional claims adjusters or law firms.
Expert Bill Review Witnesses
NRU provides experienced and knowledgeable expert witnesses who will demonstrate creative defense strategies proven to be successful. Our expert witnesses assist clients in coordinating tactics with defense counsel in order to achieve desired results. NRU expert bill review witnesses are available at competitive rates.
Extensive research completed prior to any settlement negotiation helps uncover loopholes, which helps prepare a solid defense strategy. This is also when we determine if bringing in an industry expert would benefit the negotiation.
- Our team includes expert negotiators, hearing reps and expert witnesses
- Industry recognized experts with available testimony and references
- Litigation vs. settlement analysis
- Documented results
Negotiating Saves Our Clients Money
- Less expensive than litigation
- Thorough front–end investigations eliminate file re–opens
- Lower defense costs on your files
- Reduced spending on medical files
- Increased cost savings due to more aggressive settlements
- Ability to perform bulk settlements with lien claimants
- Faster file closure and files remain closed
- Fully customizable solutions tailored to your needs
- Flexible claim referral processes
- Fraud and abuse detection and tracking services
- Realize your savings goals and impact your bottom line
Lien Resolution Pricing
- Negotiated savings below Official Medical Fee Schedule
- Negotiated savings below total lien amount for OMFS exempt liens (i.e. interpreting liens)
Fees for negotiation services are based on results achieved, which ensure our clients receive maximum savings.
We work closely with a Special Investigations Unit (SIU) to uncover and report suspected fraudulent or abusive activity on the part of the lien claimants.
